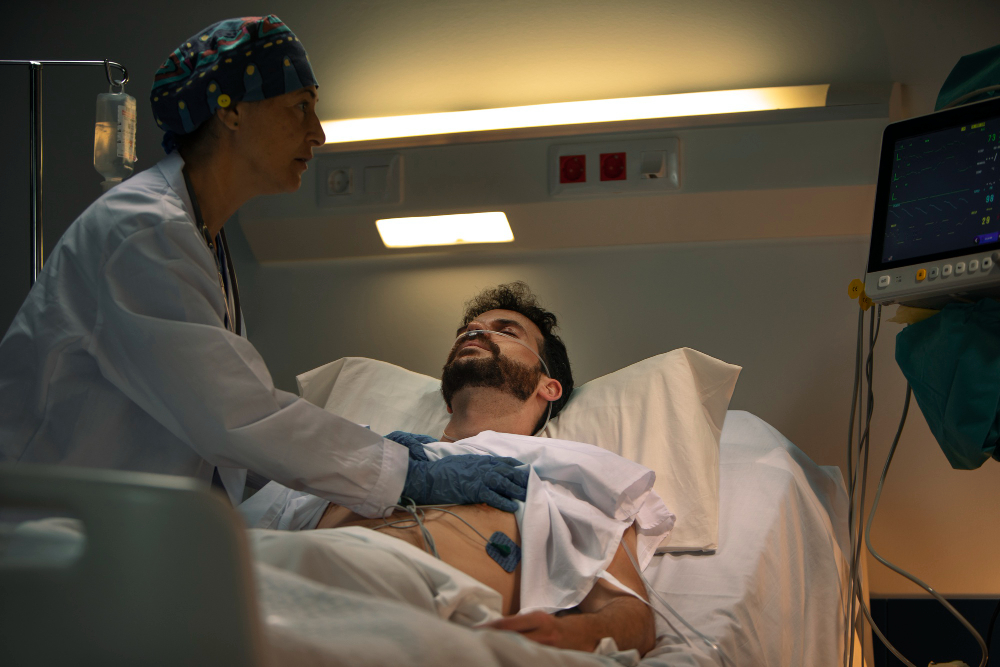
The idea of spending the night in a sleep laboratory, connected to sensors and observed remotely, can feel intimidating at first. Many people imagine a cold clinical space and an uncomfortable experience that makes sleep impossible. In practice, the reality is very different and far more reassuring. Polysomnography, often referred to as PSG, is the most detailed and reliable method available for diagnosing sleep disorders. This article explains exactly what happens during an in-clinic sleep study, guiding you through the entire process from arrival in the evening to leaving refreshed the next morning.
Why is polysomnography the gold standard?
Polysomnography is considered the gold standard because it captures a complete and synchronised picture of sleep. Unlike wearable devices or simplified home tests, it records brain waves, eye movements, muscle activity, breathing patterns, heart rhythm, and blood oxygen levels at the same time. This comprehensive approach allows clinicians to understand not only how long you sleep, but how well your body functions throughout the night. The depth of information gathered during a sleep study makes it essential for diagnosing complex conditions.
Disorders such as narcolepsy, REM sleep behaviour disorder, parasomnias, and certain forms of sleep apnoea cannot be reliably identified without observing neurological and physiological signals together. Polysomnography provides the clinical certainty required to make confident diagnoses and avoid inappropriate or ineffective treatment. Another reason for its status is the controlled clinical environment. Throughout the night, a trained sleep technologist monitors the recordings in real time. If a sensor becomes loose or a signal weakens, it can be corrected immediately. This level of oversight ensures data accuracy and reliability, which is vital when treatment decisions depend on precise interpretation.
Step-by-step: the night of the study
1. Arrival & check-in
Patients usually arrive at the sleep clinic during the early evening. The environment is intentionally designed to feel welcoming rather than clinical. Most sleep centres offer private bedrooms with comfortable beds, soft lighting, and an en-suite bathroom. This setting helps to create a sense of ease and familiarity, encouraging natural sleep rather than reinforcing the feeling of undergoing a medical test. Patient comfort in the sleep laboratory environment is important for obtaining quality recordings.
During check-in, the technologist explains the process clearly and answers any final questions. You are encouraged to follow your normal evening routine as closely as possible. Personal items such as nightwear, toiletries, and a book can be used just as they would be at home, supporting a relaxed transition to bedtime.
2. The hook-up
Preparation involves attaching a series of small sensors to specific areas of the body. These include adhesive pads on the scalp, face, chest, and legs, as well as elastic belts around the chest and abdomen to measure breathing effort. A small clip is placed on the finger to monitor oxygen levels throughout the night. The sensors are non-invasive and painless. While they may feel unusual at first, they do not restrict movement. You can turn over, adjust your position, and sleep in your usual posture. The aim is to observe typical sleep behaviour, not to force stillness or discomfort.
3. Lights out and monitoring
Once preparation is complete, the lights are turned off at your usual bedtime. From a separate control room, the technologist monitors the signals and video feed discreetly. Their role is supportive rather than intrusive, ensuring recordings remain accurate while respecting privacy. A common concern is the fear of not being able to sleep. This is entirely expected. Importantly, a full eight hours of uninterrupted sleep is not required. Even shorter periods provide enough data for meaningful analysis, as the study focuses on quality and patterns rather than duration alone.
4. The morning after
In the morning, you are gently awakened, and the sensors are removed. This process usually takes around ten minutes. There is no recovery period required, and most people feel well enough to continue with their normal day. Many patients head straight to work or return home with minimal disruption to their routine. The collected data is then analysed in detail by sleep specialists. Results are reviewed carefully, and a follow-up appointment is arranged to discuss findings and next steps. The overnight experience itself is complete, but it forms the foundation for long-term improvement in sleep health.
What exactly are we measuring?
Brain wave activity is recorded using electroencephalography, allowing clinicians to identify sleep stages accurately. These stages include light sleep, deep restorative sleep, and rapid eye movement sleep. Understanding how often you enter each stage, and how long you remain there, helps explain symptoms such as persistent fatigue or poor concentration. Breathing patterns and oxygen levels are measured continuously throughout the night. This information is crucial for identifying breathing disturbances, including obstructive and central sleep apnoea. Oxygen data reveals how significantly breathing interruptions affect the body and whether intervention is required to reduce long-term health risks.
Muscle activity sensors detect abnormal movements during sleep. These recordings help to diagnose conditions such as restless legs syndrome and periodic limb movement disorder. At the same time, heart rhythm is monitored using electrocardiography, enabling clinicians to identify sleep-related irregularities that may not appear during daytime testing.
Frequently asked questions (FAQs)
Can I use the bathroom during the study?
Yes. If you need to use the bathroom, the sleep technologist will temporarily disconnect one of the monitoring devices, and you will be free to go. Once you return to bed, the sensors are reconnected, and the study continues without affecting data quality. Staff remain available throughout the night to provide assistance promptly and discreetly.
Can I bring my own pillow or pyjamas?
Yes, absolutely. You are encouraged to bring your own pillow, pyjamas, or any personal items that help you feel comfortable and sleep more naturally. Maintaining usual bedtime habits helps to promote more natural sleep, which improves the accuracy and relevance of the recorded information. You may also follow your typical pre-sleep routine, such as reading quietly before lights out.
Can I take my regular medications?
In most cases, yes. You should continue taking your usual medications unless advised otherwise. However, it is important to inform the doctor or sleep team in advance, as some medications may affect sleep or test results. Accurate documentation ensures that results are interpreted correctly and safely within your individual medical context, supporting reliable diagnosis and appropriate treatment recommendations
Ready to get answers?
Living with untreated sleep problems can affect every aspect of daily life. Persistent sleep disruption may lead to reduced productivity, impaired memory, and difficulty maintaining focus. Over time, these effects can contribute to increased stress levels and reduced overall quality of life. Polysomnography offers clarity when symptoms remain unexplained by providing objective, clinically reliable evidence. This detailed assessment allows clinicians to identify the underlying cause of sleep disturbances accurately, ensuring that treatment recommendations are targeted, appropriate, and based on measurable data rather than assumptions.
Fear of the process is understandable, but it should not prevent access to high-quality care. In-clinic sleep studies are designed to balance comfort with clinical accuracy. Do not allow uncertainty to delay improvement. Booking a sleep study is a proactive step towards better rest, improved health, and informed treatment decisions.