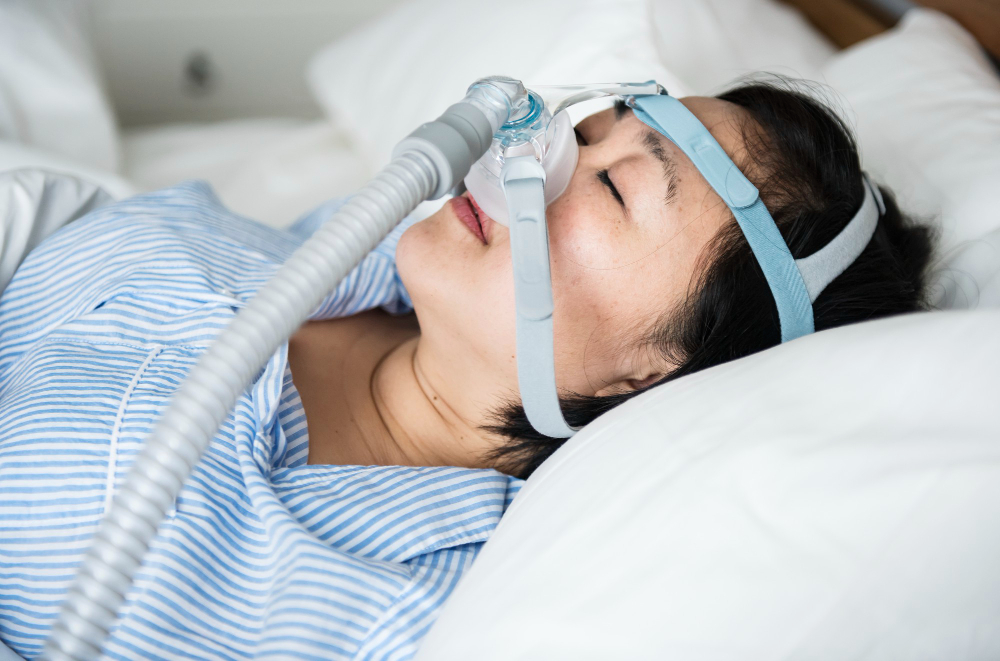
Diagnosing a serious sleep disorder once required spending an entire night in a specialised clinic under observation. Today, technological advancements enable many patients to initiate their assessment in the comfort of their own homes. A home sleep apnoea test, commonly known as HSAT, is a simplified diagnostic method designed specifically to identify obstructive sleep apnoea. While this approach offers convenience and reduced costs, it is not suitable for every individual. This article will discuss how HSAT works, who it is most suitable for, its advantages and limitations, and how it compares with in-lab sleep studies, helping you decide whether it is the right diagnostic option for your situation.
How does a home sleep test work?
A home sleep test relies on a compact medical device designed for overnight monitoring. Most systems include a small recording unit, a finger probe to measure oxygen saturation, and sensors placed on the chest to track breathing patterns. Some services use advanced technology such as WatchPAT, which estimates sleep behaviour through changes in peripheral arterial tone. These components are lightweight and minimally intrusive, allowing sleep to occur in a familiar environment without major disruption.
The testing process is intentionally simple to encourage correct use. After confirming suitability, the patient either collects the device from a clinic or receives it by post. Clear instructions explain how to apply the sensors before bedtime. The test is worn for one night only, after which the equipment is returned for analysis, ensuring minimal impact on daily routines or work commitments. During sleep, the device records oxygen levels, heart rate, airflow, and snoring activity. Using this information, clinicians calculate the apnoea hypopnea index (AHI), which represents the average number of breathing interruptions per hour. This index is central to diagnosing obstructive sleep apnoea and determining its severity according to recognised clinical thresholds.
The benefits of testing at home
Comfort is one of the strongest advantages of home testing. Sleeping in one’s own bed allows individuals to follow their normal routines and avoid the anxiety often associated with clinical environments. This familiarity can lead to more natural sleep patterns, improving tolerance of the equipment and supporting reliable data collection. Cost effectiveness is another important benefit. HSAT is typically far less expensive than an in-laboratory sleep study, as it requires less equipment and staffing. For patients without full insurance coverage, this affordability can remove a significant barrier to diagnosis and allow earlier intervention for a potentially serious condition. Home testing also improves accessibility. Patients with mobility limitations, caring responsibilities, or limited access to specialist centres may find overnight hospital stays difficult. HSAT removes the need for travel and overnight absence, making diagnostic assessment more achievable and encouraging timely evaluation.
Who is eligible for a home test?
Home sleep apnoea testing is best suited to a clearly defined group of patients. The ideal candidate is an adult with symptoms strongly suggestive of obstructive sleep apnoea, such as loud snoring, witnessed breathing pauses, or excessive daytime sleepiness. Screening tools like the STOP-BANG questionnaire help clinicians identify individuals with a high probability of moderate to severe disease. Eligibility also depends on medical history. Patients should not have significant heart, lung, or neurological conditions that could affect breathing during sleep. HSAT is designed for targeted diagnosis rather than comprehensive sleep evaluation, making appropriate patient selection essential for accurate results.
Patients must also be able to manage the equipment independently. Correct placement of sensors is necessary for meaningful data collection. Individuals who can follow instructions and feel comfortable using simple medical devices are more likely to achieve high-quality recordings and clinically useful outcomes.
Who should not do a home test? (the limitations)
HSAT has important diagnostic limitations. It cannot identify complex sleep disorders such as narcolepsy, restless legs syndrome, or parasomnias. These conditions require monitoring of brain activity and muscle movement, which home devices do not measure. Patients with unusual or unexplained symptoms require laboratory-based testing. Certain medical comorbidities also limit suitability. Individuals with heart failure, severe chronic lung disease, or neuromuscular conditions may have breathing abnormalities that HSAT cannot reliably assess. In these cases, laboratory studies provide the level of monitoring required for accurate diagnosis and patient safety.
HSAT is also less effective for people with significant insomnia. If sufficient sleep is not achieved, the test may fail to collect usable data. Additionally, because the device cannot distinguish wakefulness from sleep, it may underestimate disease severity. Ongoing symptoms despite a negative result should prompt further investigation.
HSAT vs. in-lab study: a quick comparison
The differences between home sleep testing and laboratory studies are important when selecting the most appropriate diagnostic approach. The table below highlights the key distinctions in scope, accuracy, and convenience to support informed clinical decision making.
| Feature | Home sleep apnoea test (HSAT) | In-lab sleep study (Polysomnography) |
| Monitoring scope | Measures breathing patterns and oxygen saturation only | Measures brain activity, sleep stages, muscle movement, heart rhythm, and breathing |
| Conditions diagnosed | Diagnoses obstructive sleep apnoea only | Diagnoses all sleep disorders |
| Accuracy level | High accuracy for uncomplicated obstructive sleep apnoea | Highest diagnostic accuracy across all sleep conditions |
| Testing environment | Conducted at home in the patient’s own bed | Conducted overnight in a specialised sleep laboratory |
| Convenience | Very high convenience with minimal disruption | Lower convenience due to overnight clinical attendance |
| Best suited for | Patients with a high likelihood of moderate to severe OSA | Patients with complex symptoms or unclear diagnoses |
What happens after the test?
Once the test is completed, the recorded data is reviewed by a qualified sleep specialist. Automated analysis supports the process, but professional interpretation remains essential. The clinician evaluates the apnoea hypopnea index alongside oxygen levels and reported symptoms to confirm or exclude obstructive sleep apnoea. If the test is positive, appropriate treatment options are discussed, often beginning with continuous positive airway pressure therapy. If results are negative but symptoms persist, an in-laboratory study may be recommended to ensure no underlying condition has been missed.
Start your journey from home
Persistent snoring, daytime fatigue, and reduced concentration should not be ignored. For eligible patients, a home sleep apnoea test offers a practical and accessible starting point for diagnosis. Contacting a qualified provider allows assessment of suitability and timely access to appropriate care without unnecessary disruption. For those uncertain about their symptoms, understanding the difference between simple snoring and sleep apnoea is an important step. Reliable information and specialist guidance support informed decisions, helping patients move confidently towards improved sleep health and long-term wellbeing. Contact us to see if you qualify for a home sleep apnoea test.